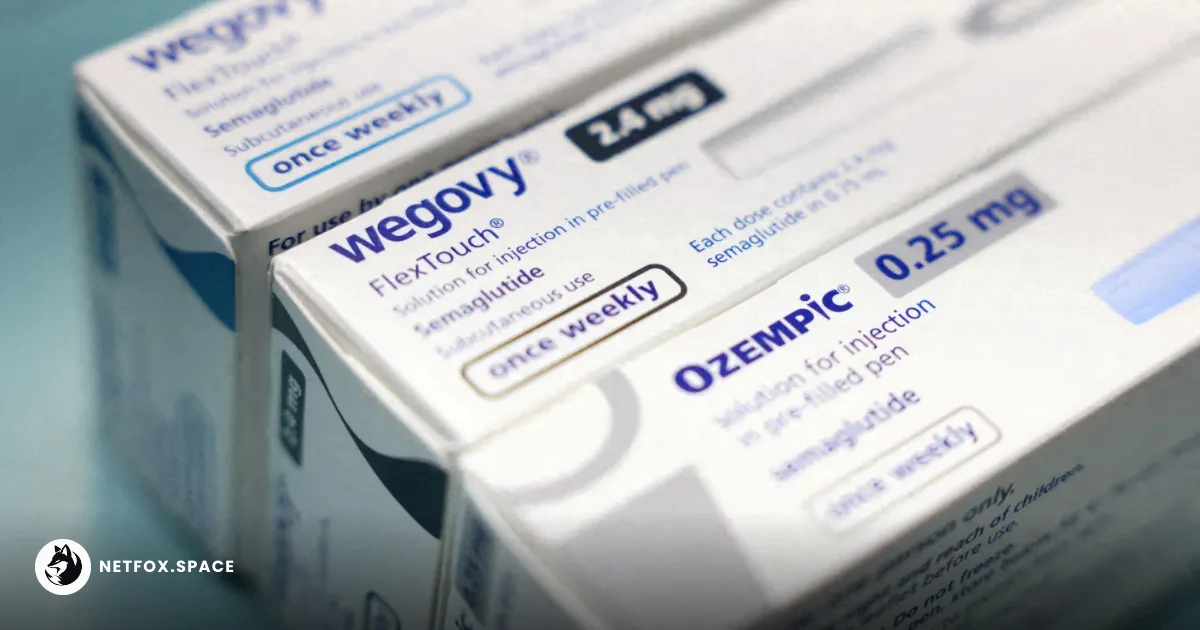
Clinical Findings on Post-Treatment Cardiac Events
Recent clinical data released on March 18, 2026, highlights a critical vulnerability for patients who cease using Glucagon-like peptide-1 (GLP-1) receptor agonists. The study indicates that individuals who stop taking medications such as semaglutide or tirzepatide face a measurable increase in the incidence of myocardial infarction (heart attack), stroke, and all-cause mortality.
Researchers observed that the protective cardiovascular benefits associated with these drugs often used to treat type 2 diabetes and obesity diminish rapidly once the biological signaling is interrupted. This shift suggests that the metabolic stabilization provided by the biopharmaceutical sector's leading weight-loss drugs may not offer a "legacy effect" once the patient defaults on their regimen.
Immediate Physiological Rebound and Metabolic Instability
The cessation of GLP-1 therapy triggers an immediate shift in glycemic control and blood pressure regulation. For many patients, the rapid return of appetite and subsequent weight regain contributes to an acute spike in systemic inflammation. This physiological "rebound" places immense strain on the cardiovascular system, particularly in patients with pre-existing atherosclerotic conditions.
Medical professionals are observing that the sudden withdrawal of these peptides can lead to a surge in proinflammatory cytokines. This chemical shift often correlates with the destabilization of arterial plaques, which is a primary precursor to the life-threatening strokes and heart attacks identified in the latest research.
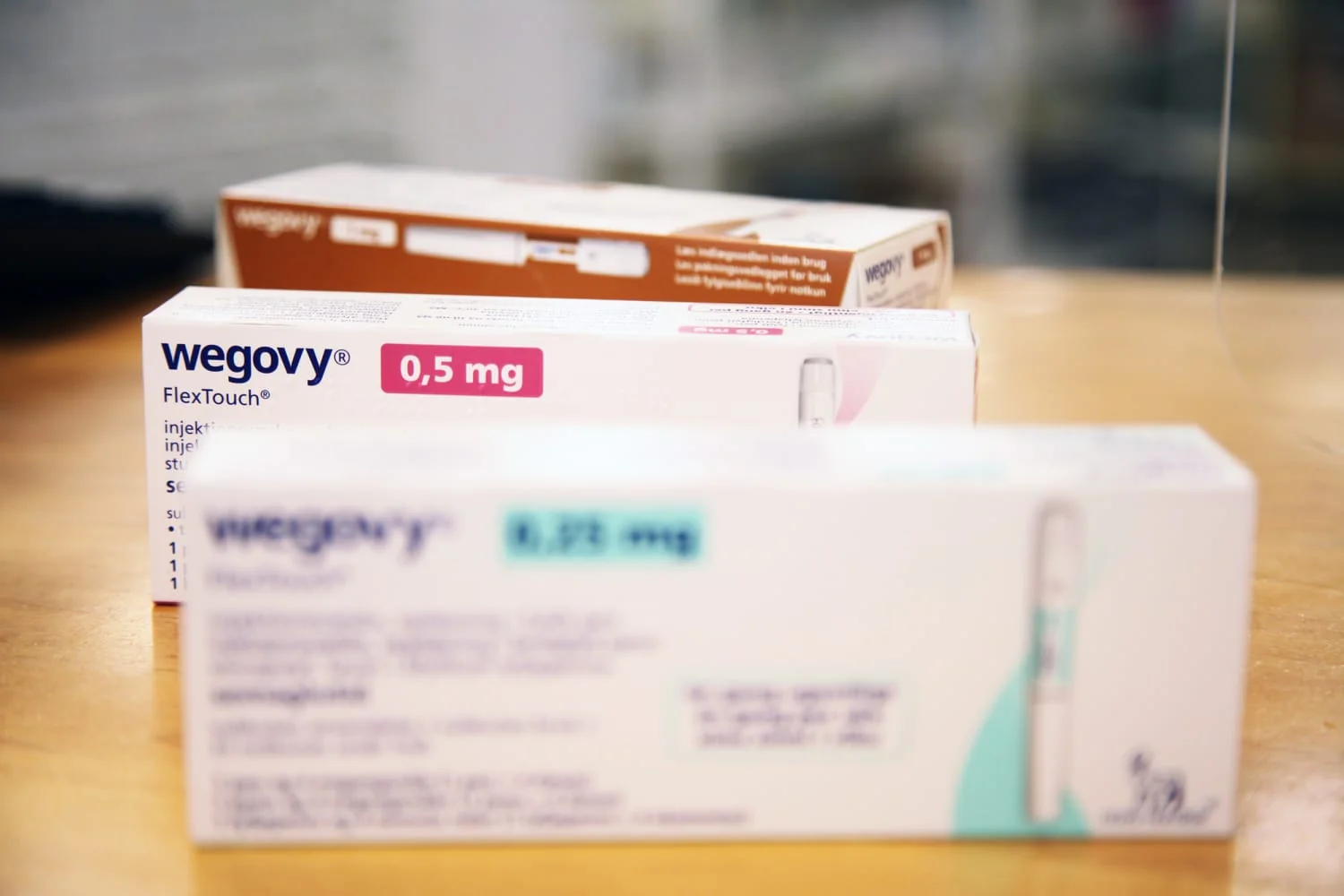
The "Biological Tether" and Long-Term Dependency
While most reporting focuses on the return of weight, the underlying "biological tether" created by GLP-1s is the more significant clinical concern. These drugs do not "cure" metabolic dysfunction; they manage it by modulating the incretin system. When the drug is removed, the body’s natural metabolic sensors often already compromised cannot maintain the artificial equilibrium previously established.
This creates a structural shift in how chronic disease must be managed. The medical community must now view GLP-1s not as a temporary intervention, but as a potential life-long requirement for cardiovascular stability. The "hidden implication" is that discontinuing the drug may be more dangerous for a patient's heart health than never having started it at all, due to the rapid fluctuations in vascular pressure and lipid profiles during the withdrawal phase.
Systemic Pressure on Healthcare Payers and Insurance
The findings place the healthcare insurance industry and government programs like Medicare in a complex regulatory position. If stopping the medication leads to high-cost emergency room visits for strokes and heart attacks, the "cost-saving" measure of limiting GLP-1 coverage becomes a long-term financial liability.

Cardiovascular Risk Comparison: Active vs. Discontinued Use
| Metric | Active GLP-1 Therapy | Discontinued Therapy (6-12 Months Post) |
|---|---|---|
| Systolic Blood Pressure | Generally Decreased | Significant Rebound / Increase |
| HbA1c Levels | Stabilized | Rapid Elevation |
| Inflammatory Markers (CRP) | Lowered | Acute Spike Potential |
| Risk of Major Cardiac Event | Reduced (approx. 20%) | Elevated above baseline |
The Future of Chronic Obesity Management
As the U.S. Food and Drug Administration (FDA) and international regulatory bodies review these safety signals, the narrative around "exit strategies" for weight loss drugs is changing. Clinical guidelines are likely to be updated to include strict tapering protocols rather than abrupt cessation.
The focus is shifting toward "maintenance dosing" models, where patients remain on sub-therapeutic levels of the drug to preserve cardiovascular integrity. This ensures that the metabolic "floor" does not drop out from under the patient, preventing the acute vascular shocks that lead to the reported deaths.
The looming uncertainty remains whether global healthcare infrastructures can sustain the cost of permanent, multi-decade GLP-1 prescriptions for millions of citizens, or if a secondary crisis of "uninsured withdrawal" will lead to a predictable wave of cardiovascular emergencies in the coming decade.


Comments (0)
Please login to comment
Sign in to share your thoughts and connect with the community
Loading...