Clinical Breakthrough in Breast Reconstruction Safety
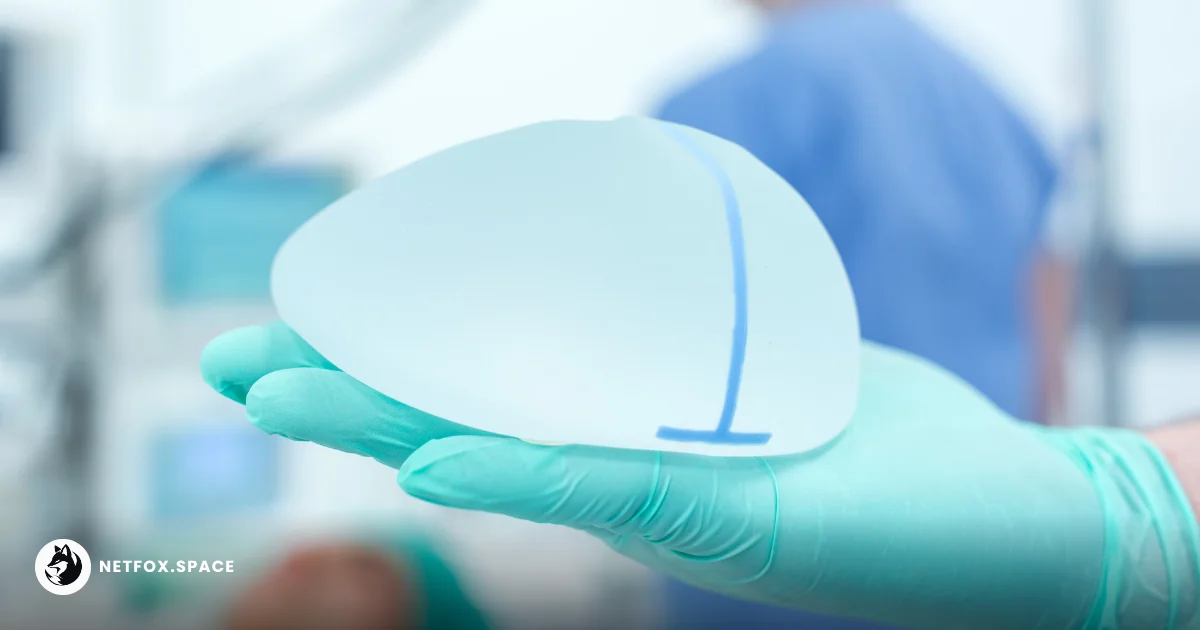
A landmark study has identified polyurethane-coated implants as a superior alternative to traditional smooth or textured silicone surfaces for patients undergoing mastectomy. Researchers found that this specific material significantly mitigates the risk of common post-operative complications that frequently lead to revision surgeries.
The data indicates a sharp decline in the incidence of infections and hematomas among breast cancer survivors. By utilizing a foam-like surface, these implants integrate more effectively with the surrounding biological tissue, preventing the mechanical friction that often triggers inflammatory responses.
 Credit: Unsplash/CC0 Public Domain
Credit: Unsplash/CC0 Public Domain
Mitigation of Capsular Contracture Risks
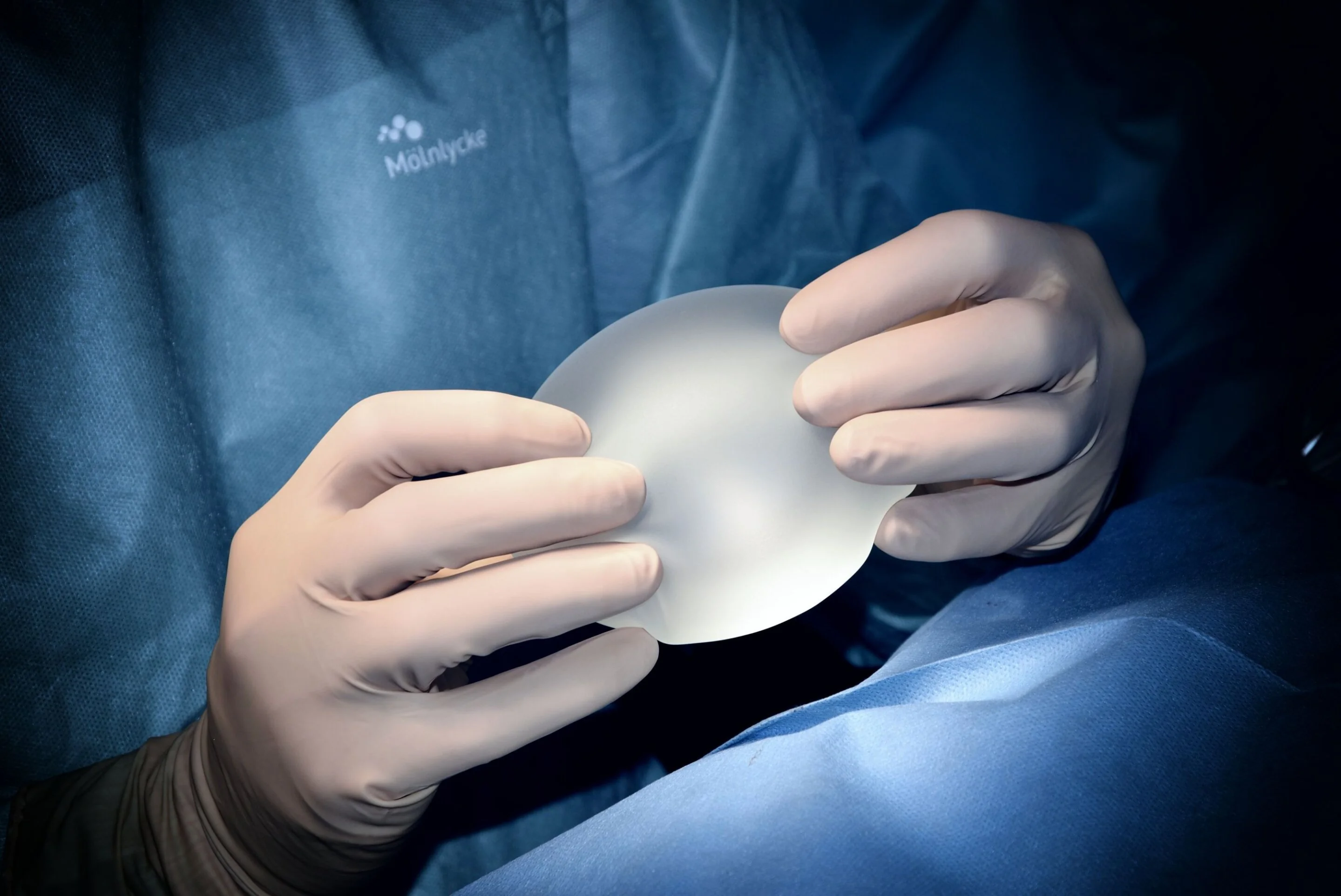
The most significant finding centers on the reduction of capsular contracture, a painful condition where scar tissue tightens around the foreign object. Traditional silicone implants often trigger a "foreign body response" that leads to hardening and distortion of the breast area.
The polyurethane layer acts as a scaffold, allowing microscopic tissue ingrowth that breaks up the formation of linear collagen fibers. This structural interference prevents the development of a thick, constrictive capsule, maintaining the aesthetic and functional integrity of the reconstruction over a longer duration.
The Biomechanical Mechanism: Why Surface Geometry Matters
While most discussions focus on the chemical composition of implants, the true differentiation lies in the "micro-environment" created by the polyurethane foam. Unlike textured silicone, which provides a macro-surface for grip, the polyurethane structure creates a three-dimensional porous matrix.
This matrix traps individual fibroblasts, the cells responsible for collagen production, forcing them to deposit tissue in a multidirectional, non-linear fashion. By preventing the alignment of these cells, the material mathematically reduces the contractile force the scar tissue can exert on the implant. This mechanical "disarming" of the body's immune response is a critical shift from passive biocompatibility to active tissue integration.
 Credit: Getty Images
Credit: Getty Images
Economic and Systemic Shifts in the Biotech Sector
The adoption of polyurethane-coated technology represents a significant pivot for the medical device industry. While these implants are historically more expensive than standard silicone options, the reduction in secondary "salvage" surgeries presents a compelling case for healthcare payers and insurance providers.
Hospital systems are increasingly scrutinizing long-term outcomes to reduce the "re-admission burden" associated with reconstructive failure. As clinical evidence mounts, regulatory bodies like the European Medicines Agency and global health departments may re-evaluate procurement standards, favoring materials that demonstrate lower lifetime intervention rates.
Comparative Risk Profile of Implant Surfaces
| Feature | Smooth Silicone | Textured Silicone | Polyurethane Coated |
|---|---|---|---|
| Tissue Adhesion | Low | Moderate | High (Bio-integration) |
| Capsular Contracture | Higher Risk | Variable | Lowest Documented Risk |
| Displacement Risk | High (Rotation) | Moderate | Minimal (Velcro-effect) |
| Primary Benefit | Soft Feel | Stability | Long-term Safety |
Escalating Scrutiny of Long-Term Bio-Stability
The transition toward advanced coatings occurs as the medical community faces increasing pressure to address Breast Implant-Associated Anaplastic Large Cell Lymphoma (BIA-ALCL). While polyurethane coatings show immense promise in preventing mechanical failure, the industry must now provide granular, multi-decade data on the degradation of the foam itself over 20+ years.
The long-term chemical stability of the polyurethane-silicone bond remains a focal point for longitudinal studies, as any potential for material shedding could trigger new regulatory hurdles. Clinical focus is now shifting from immediate post-operative success to the permanent bio-stability of these complex polymer structures within the human endocrine environment.


Comments (0)
Please login to comment
Sign in to share your thoughts and connect with the community
Loading...