New clinical data from pancreatic and melanoma trials suggests that mRNA technology, once the cornerstone of the pandemic response, is finding a durable application in personalized oncology. While researchers caution that these therapies are years from standard-of-care status, the ability to trigger specific T-cell responses in patients with high-mortality cancers has shifted the focus toward individualized treatment.
Personalized neoantigen targeting drives immune durability
The shift in recent cancer vaccine research marks a departure from "off-the-shelf" vaccines toward personalized neoantigen therapy. Unlike traditional vaccines that target a universal pathogen, these mRNA candidates are designed by sequencing a patient’s specific tumor to identify unique mutations.
Early results from trials focusing on pancreatic cancer indicate that mRNA can instruct the body to produce proteins that mimic these mutations, effectively "training" the immune system to recognize and attack residual microscopic disease. From a clinical perspective, the most significant finding is the durability of the T-cell response; in some phase 1 participants, the immune system remained primed to target tumor cells years after the initial series of injections. This longevity is critical for preventing recurrence in cancers that are traditionally difficult to treat with surgery or chemotherapy alone.
 Much of Dr. Vinod Balachandran's work has focused on pancreatic tumors. Michael Prince/Memorial Sloan
Much of Dr. Vinod Balachandran's work has focused on pancreatic tumors. Michael Prince/Memorial Sloan
Pancreatic cancer trials show high-response benchmarks
Pancreatic ductal adenocarcinoma (PDAC) has historically been resistant to most forms of immunotherapy due to its "cold" tumor microenvironment, which effectively hides cancer cells from the immune system. However, ongoing trial data suggests that mRNA vaccines can successfully turn these tumors "hot."
In specific cohorts, roughly half of the patients treated with a combination of surgery, chemotherapy, and personalized mRNA vaccines showed a robust immune response. Those who responded remained cancer-free for significantly longer periods than those who did not. While this 50% response rate is high for pancreatic cancer, it also reveals a critical unknown: researchers have yet to determine why some patients' immune systems fail to activate despite receiving the same mRNA-encoded instructions. This gap suggests that the success of the platform may depend as much on the patient’s underlying immune health as the vaccine’s design.
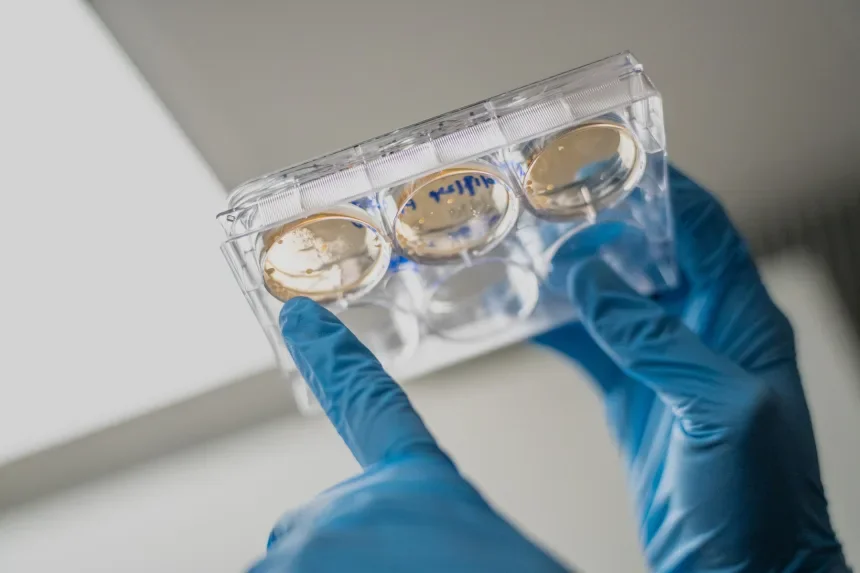 A researcher in Dr. Elias Sayour's lab examples a sample during testing. Jackie Hart/UF Health
A researcher in Dr. Elias Sayour's lab examples a sample during testing. Jackie Hart/UF Health
Logistical and manufacturing constraints limit immediate adoption
Despite the clinical optimism, the transition from successful small-scale trials to widespread clinical use faces a significant bottleneck in "vein-to-vein" time. Because each vaccine must be custom-manufactured for an individual patient, the process currently requires weeks of sequencing, design, and production.
For patients with aggressive, late-stage cancers, this delay can be prohibitive. Furthermore, the cost of individualized manufacturing remains high, raising questions about how these therapies will be integrated into public health systems. Unlike the mass-produced COVID-19 vaccines, the oncology application of mRNA requires a decentralized or highly rapid manufacturing infrastructure that does not yet exist at scale.
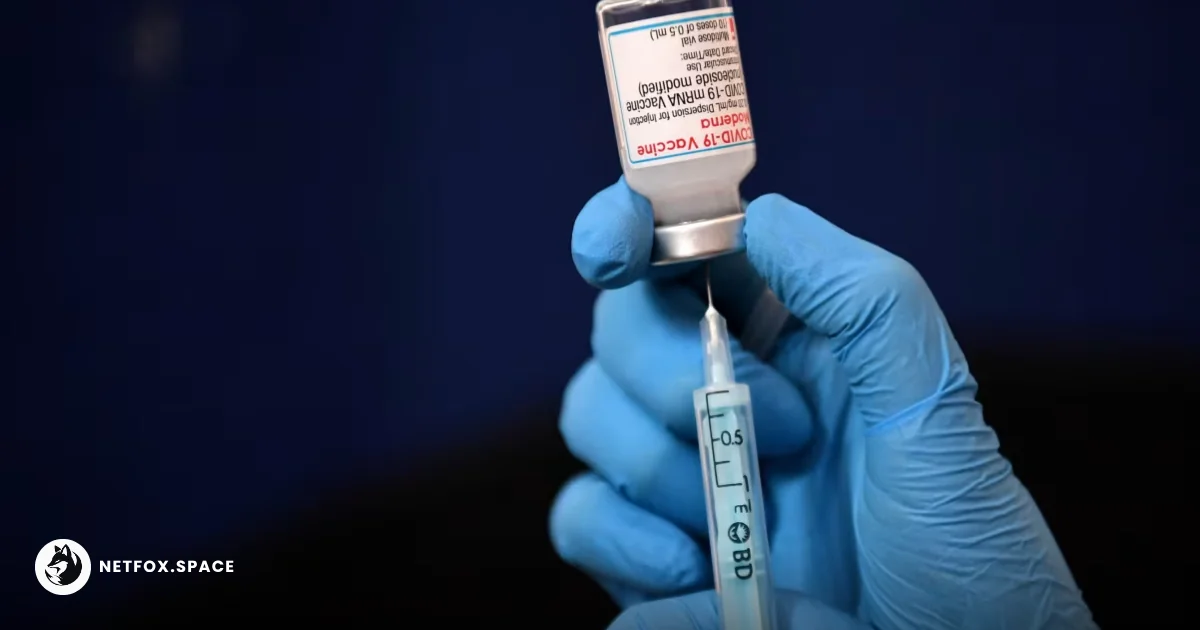
 Moderna's is one of two mRNA-based Covid-19 vaccines approved in the US. Carl Court/Getty Images
Moderna's is one of two mRNA-based Covid-19 vaccines approved in the US. Carl Court/Getty Images
Trial design shifts toward combination therapies
The current consensus among oncology researchers is that mRNA vaccines will likely not act as monotherapies. Instead, they are being positioned as a "cleanup" tool to be used alongside checkpoint inhibitors.
Checkpoint inhibitors remove the "brakes" from the immune system, while the mRNA vaccine provides the "map" of where to attack. This dual approach is being tested in larger phase 2 and 3 trials for melanoma and lung cancer. While the promising signs reported this year provide a necessary boost to the field, the industry now awaits data to prove whether these personalized responses translate into a statistically significant survival benefit across larger, more diverse patient populations.


Comments (0)
Please login to comment
Sign in to share your thoughts and connect with the community
Loading...