Scientists have finally identified the specific transport mechanism that allows Vitamin B1 to cross the mitochondrial membrane, validating a biological theory originally proposed in 1959. The discovery closes a major gap in our understanding of how cells convert nutrients into energy and why certain thiamine deficiencies manifest so aggressively in the nervous system.
Solving the mitochondrial entry problem for Thiamine
While it has been known for decades that Vitamin B1, or thiamine, is essential for cellular respiration, the precise method by which it enters the mitochondria the cell's power plants remained a theoretical mystery. In 1959, researchers hypothesized that a dedicated, high-affinity transporter must exist to move thiamine across the impermeable inner mitochondrial membrane.
Without this transport, the thiamine consumed through diet cannot reach the enzymes responsible for the citric acid cycle. The recent confirmation of this transporter's identity proves that the 1959 "crazy" theory was correct in its prediction of a bottleneck in thiamine metabolism.
 Dissolving pill
Dissolving pill
The mechanism of Thiamine Pyrophosphate transport
The research identifies a specific protein that acts as a gatekeeper, moving thiamine pyrophosphate (TPP) into the mitochondrial matrix. TPP is the active form of Vitamin B1 and serves as a critical co-factor for enzymes like pyruvate dehydrogenase.
From an operational perspective, this discovery explains why simply increasing thiamine intake does not always resolve metabolic distress; if the transporter protein is dysfunctional or absent, the mitochondria remain "starved" of the vitamin regardless of blood concentration levels. This adds a layer of complexity to treating genetic thiamine-responsive disorders, as the failure point may be the transport mechanism rather than a systemic deficiency.
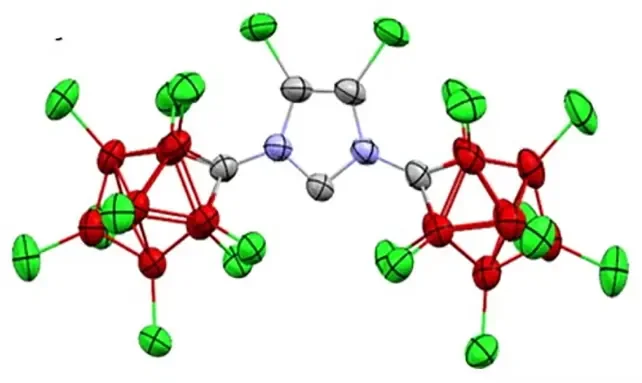 The structure of the water-stable carbene. (Lavallo Lab/UCR)
The structure of the water-stable carbene. (Lavallo Lab/UCR)
Practical implications for metabolic and neurological health
The confirmation of this 67-year-old mystery has immediate relevance for the study of Leigh syndrome and other mitochondrial encephalopathies. These conditions often mirror the symptoms of severe thiamine deficiency, such as Wernicke-Korsakoff syndrome, because both involve a breakdown in the same energetic pathway.
By isolating the specific transport protein, researchers can now investigate whether certain neurodegenerative "signals" are actually the result of localized transport failures. However, it is important to note that while the mechanism is now proven, clinical applications such as targeted gene therapies to fix these transporters remain in the early stages of laboratory validation.
Limitations of the current discovery
While the identification of the transporter is a milestone, it does not yet explain the full regulatory environment of mitochondrial thiamine. It remains unclear how the cell signals the transporter to increase activity during periods of high metabolic demand or how environmental toxins might inhibit this specific gatekeeper.
Furthermore, the study confirms the existence and identity of the transporter but does not provide a "cure" for thiamine-related pathologies. Instead, it provides a confirmed map for future pharmacology to target, shifting the focus from broad supplementation to the precise molecular mechanics of nutrient delivery at the organelle level.


Comments (0)
Please login to comment
Sign in to share your thoughts and connect with the community
Loading...