Taking Vitamin D beyond recommended levels creates a physiological paradox where excessive amounts of the "sunshine vitamin" can actively damage bone density and cardiovascular health. While essential for calcium absorption, high-dose supplementation often triggers hypercalcemia, leading to systemic complications that offset any potential gains.
The U-Shaped Curve of Vitamin D Efficacy
Clinical evidence suggests that Vitamin D does not follow a linear benefit model; instead, it operates on a U-shaped curve where both deficiency and excess lead to poor health outcomes. While the nutrient is critical for skeletal integrity, prolonged intake exceeding 4,000 IU per day for healthy adults can lead to toxicity.
Physiologically, Vitamin D's primary role is to facilitate the absorption of calcium in the gut. When levels become excessive, the body is flooded with more calcium than it can effectively manage or store in the bone matrix. This state, known as hypercalcemia, forces the mineral into soft tissues, including the kidneys and blood vessels, potentially leading to stones and vascular calcification.
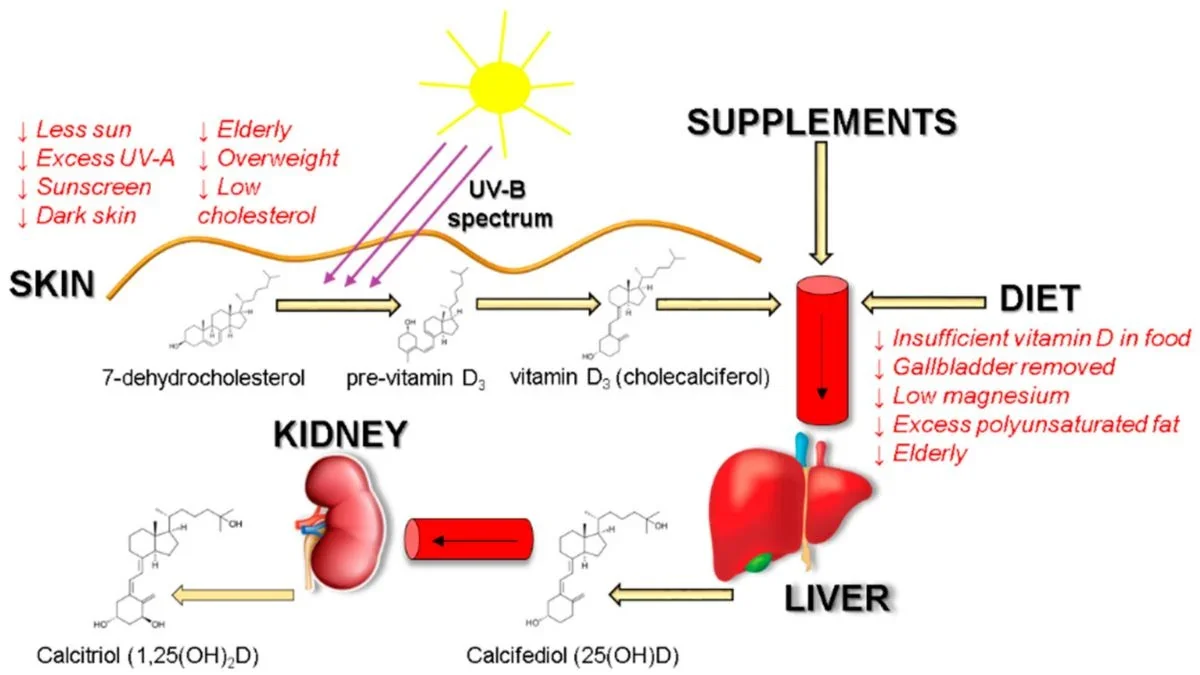 Sources of Vitamin D and possible factors affecting its absorption. Diet and lifestyle factors with downward arrows are associated with decreased vitamin D absorption and biosynthesis. (Šimoliūnas et al., Medicina, 2019)
Sources of Vitamin D and possible factors affecting its absorption. Diet and lifestyle factors with downward arrows are associated with decreased vitamin D absorption and biosynthesis. (Šimoliūnas et al., Medicina, 2019)
The Counterintuitive Risk of Increased Bone Fractures
One of the most significant findings in recent clinical reviews is the paradox regarding bone density. While many consumers take high-dose supplements to prevent osteoporosis, extreme levels of Vitamin D may actually accelerate bone resorption.
When Vitamin D levels are unnaturally high, they can over-stimulate osteoclasts the cells responsible for breaking down bone tissue. This process, intended to maintain calcium homeostasis, ends up thinning the bone it was meant to protect. This explains why some clinical trials have observed a higher incidence of falls and fractures in elderly populations taking massive annual or monthly "bolus" doses compared to those on more modest daily regimens.
 Vitamin D is known to be essential to human health — but a new study suggests that taking a certain form of it can have a negative effect. (iStock)
Vitamin D is known to be essential to human health — but a new study suggests that taking a certain form of it can have a negative effect. (iStock)
Toxicity Symptoms and Biological Limitations
Vitamin D toxicity (hypervitaminosis D) is particularly insidious because it is fat-soluble, meaning the body stores excess amounts in fat tissue and the liver for long periods. Unlike water-soluble vitamins that are easily excreted, Vitamin D can remain at toxic levels for weeks after supplementation stops.
The early markers of toxicity are often non-specific, including nausea, fatigue, and frequent urination. However, the long-term risk involves the kidneys. Because the kidneys are responsible for filtering excess calcium, hypercalcemia often manifests as nephrocalcinosis, where calcium deposits physically damage the organ's structural integrity.
 More research is needed to determine whether vitamins D2 and D3 affect the body differently — and whether that could change doctors’ medical advice on which type to take, the researchers concluded. (iStock)
More research is needed to determine whether vitamins D2 and D3 affect the body differently — and whether that could change doctors’ medical advice on which type to take, the researchers concluded. (iStock)
Distinguishing Deficiency Correction from General Wellness
A critical point of confusion for consumers is the difference between treating a diagnosed deficiency and maintaining wellness. For an individual with clinically low blood levels (typically below 20 ng/mL), high doses may be medically necessary for a short duration.
However, for those with normal levels, adding aggressive supplementation provides no documented "boost" to the immune system or mood that outweighs the risk of hypercalcemia. Practitioners emphasize that for the general population, the Recommended Dietary Allowance (RDA) of 600 to 800 IU remains the safest benchmark, as the body’s natural regulatory systems for Vitamin D primarily through skin exposure to UV light are designed to prevent the very toxicity that synthetic supplements can easily bypass.


Comments (0)
Please login to comment
Sign in to share your thoughts and connect with the community
Loading...